- Home
- Research
- Research Centres and Laboratories
- JC STEM Lab of Innovative Light Therapy for Eye Diseases
- Dry Eye
- Intense Pulsed Light Therapy for Dry Eye Disease
Intense Pulsed Light Therapy for Dry Eye Disease
(https://www.eyelink.com/eye-care-services/dry-eye-optometrist/dry-eye-treatments/intense-pulsed-light-therapy-ipl/)
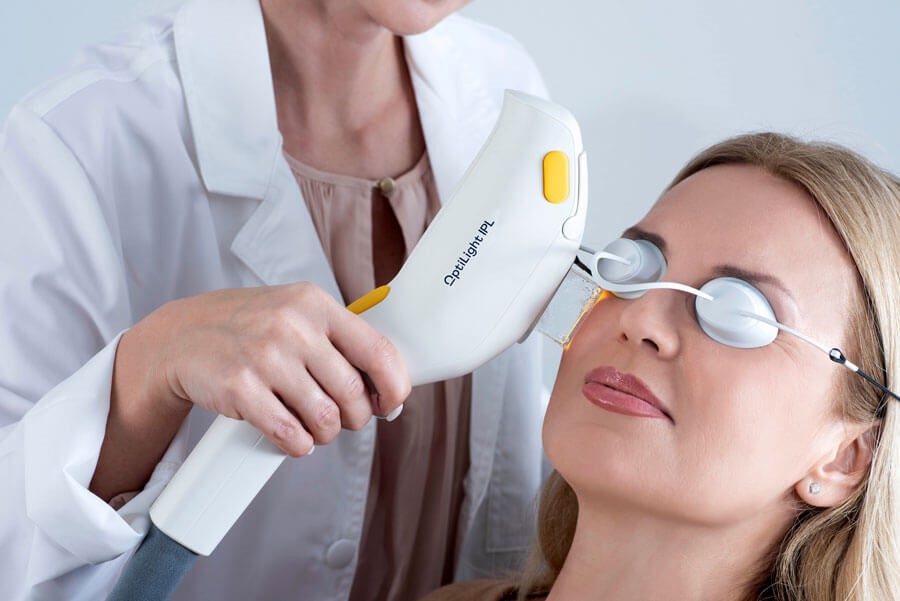
Dry eye disease (DED) is a prevalent condition that can significantly impact patients' quality of life, causing discomfort, pain, and visual disturbances. Traditional treatments, such as eye drops and warm compresses, offer temporary relief but often fail to address the root cause. In recent years, Intense Pulsed Light (IPL) therapy has emerged as a promising treatment option for meibomian gland dysfunction(MGD), which is an important factor causes DED, offering a potential long-term solution for patients suffering from this chronic condition.[1]
How IPL Works: Unraveling the Mechanisms
IPL therapy utilizes high-intensity, polychromatic, non-coherent light pulses to target specific chromophores in the skin, such as hemoglobin and melanin. The light energy absorbed by these chromophores is converted into heat, leading to a photothermal effect that helps in the treatment of various skin conditions, including dry eye syndrome.
In the context of dry eye treatment, IPL targets the meibomian glands, which are responsible for producing the lipid layer of the tear film. The heat generated by IPL can help liquefy and release the hardened meibum, improving gland function and reducing inflammation. Additionally, IPL can induce intravascular thrombosis in telangiectatic blood vessels, reducing the inflammatory mediators' access to the meibomian glands.[2](Fig1. Meibomian Gland Dysfunction)
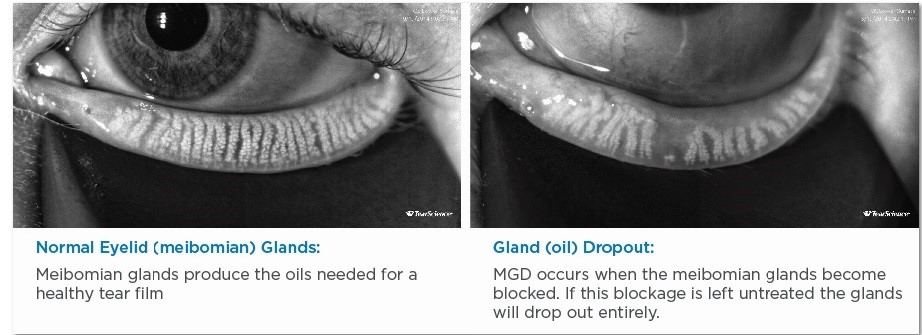
Fig1. Meibomian Gland Dysfunction
(https://www.eyelink.com/eye-care-services/dry-eye-optometrist/dry-eye-treatments/intense-pulsed-light-therapy-ipl/)
Efficacy: The Evidence Supports Positive Outcomes
Clinical studies have demonstrated IPL's efficacy in improving dry eye symptoms and meibomian gland function. A retrospective study conducted at the Mayo Clinic and published in Cornea in 2016 showed that 58% of patients experienced a significant reduction in dry eye symptoms after IPL treatment[3]. Similarly, a study featured on EyeWiki reported that IPL therapy increased tear film stability and reduced meibum viscosity, leading to improved ocular comfort[4]. A systematic review shows significant improvements after IPL therapy, in tear film stability, meibomian gland functionality, and patient-reported outcomes such as the Ocular Surface Disease Index (OSDI) and Standard Patient Evaluation of Eye Dryness (SPEED) questionnaire scores. In addition, IPL therapy has been found to be particularly effective in patients with MGD and those with increased tear evaporation due to blocked oil glands[5].
Safety: A Relatively Well-Tolerated Procedure
IPL therapy is considered safe when performed by trained clinicians, with appropriate protective measures in place. The procedure is FDA-approved and has been shown to have a favorable safety profile in numerous clinical studies[6]. It is generally well-tolerated, with mild and transient side effects such as eyelid redness, swelling, and a sensation of heat during the procedure. Rarely, patients might experience more severe reactions like corneal abrasion or changes in skin pigmentation[7]. However, these risks can be minimized with proper patient selection, careful treatment parameter adjustment, and the use of protective eye shields during the procedure.
Case Studies: Real-World Applications
Dr. Wu, a dry eye specialist, shared his experience with OptiLight IPL treatment on the Silicon Valley Eye Physicians website[8]. He reported a significant reduction in dry eye symptoms, including scratchiness, sandiness, and grittiness, after the first session. His story is not unique; many patients have reported improved quality of life following IPL treatment.
Availability: Bringing IPL to Your Clinic
IPL therapy is increasingly being adopted by ophthalmology clinics and optometrists' offices worldwide, making it a convenient treatment option for patients. The treatment is typically administered in a series of sessions, with each session spaced a few weeks apart. The total number of sessions required varies depending on the severity of the dry eye condition.
However, its availability may vary depending on geographical location and insurance coverage. While the treatment is FDA-approved and has shown promising results, it is not covered by insurance, which may pose a financial burden for some patients[9]. Despite this, many patients find the relief from symptoms achieved through IPL therapy to be worth the out-of-pocket expense.
Conclusion: A New Frontier in Dry Eye Treatment
Intense Pulsed Light therapy offers a novel, effective, and relatively safe treatment option for patients suffering from DED, particularly those with MGD. By targeting the underlying cause of evaporative dry eye, IPL has the potential to provide long-lasting relief and improve patients' quality of life. As clinical experience grows and further studies elucidate the long-term efficacy and optimal treatment protocols, IPL is likely to become an increasingly important tool in the clinician's arsenal against dry eye disease.
References
1. Jones, L., et al., TFOS DEWS III Management and Therapy Report. American Journal of Ophthalmology, 2025.2. Gupta, A.S., M. Massaro, and V.Y. Bunya, Intense pulsed light treatment for the management of meibomian gland dysfunction. Curr Opin Ophthalmol, 2024. 35(4): p. 322-328.
3. Shen, J. F., Vegunta, S., Patel, D., & Mayo Clinic Dry Eye Clinic Research Team.Combination therapy of intense pulsed light therapy and meibomian gland expression (IPL/MGX) can improve dry eye symptoms and meibomian gland function in patients with refractory dry eye: A retrospective analysis. Cornea, 2016.35(7), 318-322.
4. Wladis, E.J., et al., Intense Pulsed Light for Meibomian Gland Disease: A Report by the American Academy of Ophthalmology. Ophthalmology, 2020. 127(9): p. 1227-1233.
5. Lei, Y., et al., Intense pulsed light (IPL) therapy for meibomian gland dysfunction (MGD)-related dry eye disease (DED): a systematic review and meta-analysis. Lasers Med Sci, 2022. 38(1): p. 1.
6.https://www.icareassociates.com/blog/what-is-the-success-rate-of-ipl-for-dry-eyes-discover-the-facts-about-optilight-treatment.html
7. Papageorgiou, P., et al., Treatment of rosacea with intense pulsed light: significant improvement and long-lasting results. Br J Dermatol, 2008. 159(3): p. 628-32.
8. https://www.eyelink.com/testimonial/optilight-ipl-dry-eye-testimonial/
9. U.S. Food & Drug Administration. 510(k) Premarket Notification Database: Lumenis OptiLight. K203333. Issued 2021-07-09. Accessed 2024-02-15. https://www.accessdata.fda.gov/scripts/cdrh/cfdocs/cfpmn/pmn.cfm




